1-2-3 Device Redesign
Empowering childhood cancer and blood disease patients to reduce risk of infection rates through gamifying their daily infection prevention activities.

CUSTOMER
ROLE
Cincinnati Children's Hospital
UX Design Fellow, Researcher, & UX/UI Design Lead
TOOLS
Figma, Adobe Illustrator
SKILLS
Qualitative Research · User Testing · Iterative Design · User Interviews · Information Architecture · Data Visualization · Wireframing · Prototyping · Leadership · Project Management · Customer Collaboration & Communication · Design Thinking · Research Synthesis · Presenting
1-2-3 Device Background
The 1-2-3 initiative was developed in an effort to reduce infection rates and help patients manage physical activity and hygiene. This project was founded from a nurse-backed incentivized program that awarded stickers to patients who completed three activities of daily living (ADL’s). These ADL’s include bathing once, doing physical activity twice, and doing oral care three times hence the naming of the 1-2-3 Device.
The 1.0 device was developed to help automate this process for Bone Marrow Transplant (BMT) and Cancer/Blood Disease (CBDI) patients. Patients use the device to log these activities and keep track of points awarded for completion. RFID cards are swiped by patients for logging activities, and parents and nurses use their RFID cards to verify points.

Version 1.0 Device
The 1.0 device with family/caregiver RFID card before the redesign.
Key Problem Space
While the 1.0 device improved on overall patient adherence, it was difficult and time consuming for nurses to manage, lacked a deeper sense of patient motivation, was difficult to upkeep, and required more advanced functionality and hardware.
Project Goals

01
Understand experiential deficiencies of the 1.0 device and identify opportunities for improvement.

02
Develop a deeper understanding of what motivates patients to increase their compliance.

03
Design a V 2.0 with improved interaction, usability, and experience.
In-depth Interviews
CCH Technical Leads
CCH Project Managers
CCH Clinical Research Coordinators
CCH Nurses
Patients & Parents/ Caregivers
Research Insights
Patient and/or Family Caregivers
Looking at what patient/caregiver motivators and barriers exist for each activity.

Healthcare Professionals
Looking at what staff barriers exist for each activity of daily living

1.0 Device Interaction Map
The interaction map outlines every daily expected interaction with the 1.0 device as well as the pain points and opportunities areas for improvement. We learned that the 1.0 device requires far too much redundant interaction for nurses and families to maintain, which often left patients waiting for point gratification

Wireframing

User Testing: Part 1
Tested with 6 Patients
An avatar concept was originally proposed by nurses so it was well received when testing with staff; however when testing with older patients (teens), they felt it was too childish for them.
User Testing: Part 2
Tested with 10 Patients
While overall usability was successful, there were mainly issues with the overall concept of verifying points. Nurses felt that being part of the verification process was unnecessary due to their already large workload.
We also discovered that not every child has a consistent family member to take part in validating points. Nurse and family members were mostly concerned about the patient’s overall adherence trend rather than day-to-day interactions.
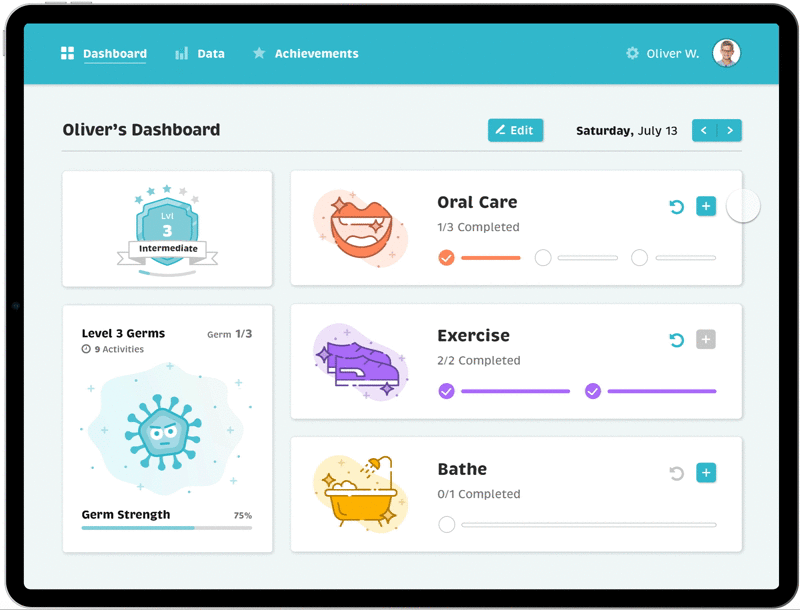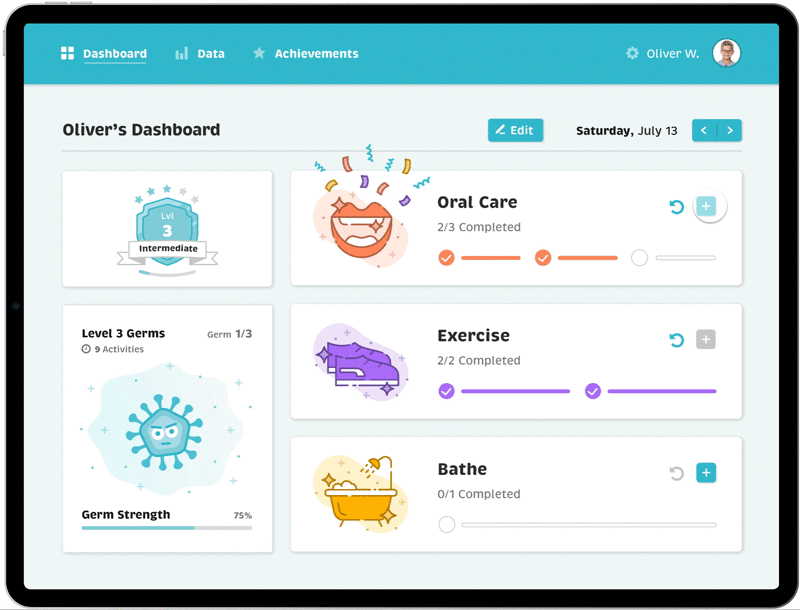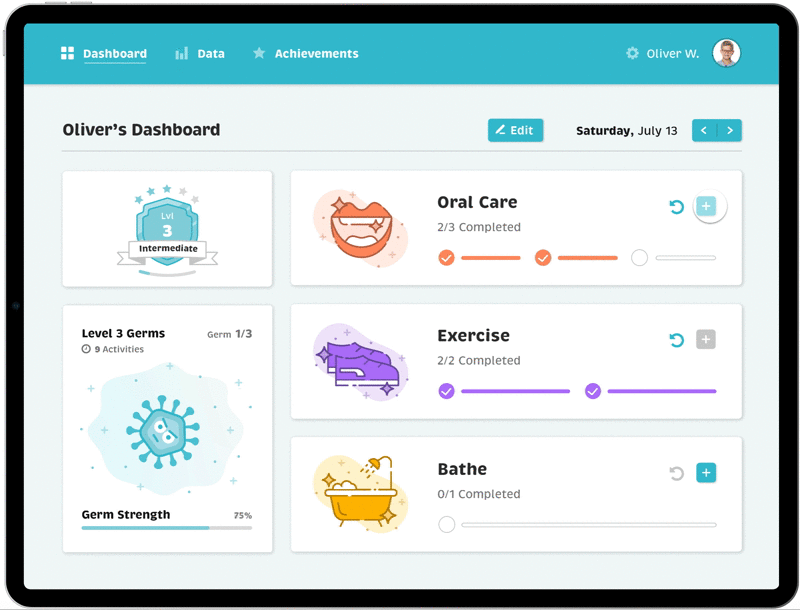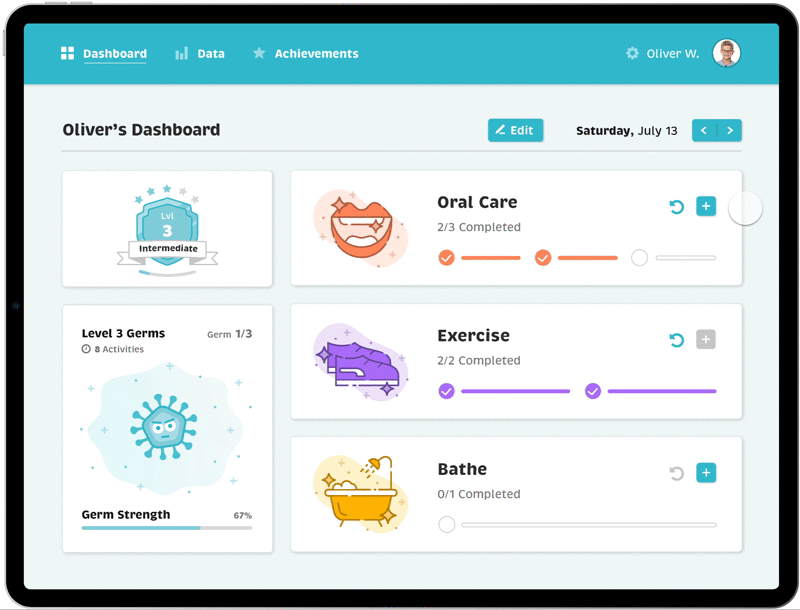
Final Designs: Activity Dashboard
Gamification of Positive
Reinforcement
Final Designs: Achievements
Final Designs: Customizing & Editing Activities
Final Designs:
Data & Progress Tracking